Translate this page into:
Management strategies for transmigrated mandibular canines: Two case reports and review of treatment options

*Corresponding author: Prema Anbarasu, Reader, Department of Orthodontics, Chettinad Dental College and Research Institute, Kelambakkam, Tamil Nadu, India. prema.arasu@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Ramesh Babu R, Anbarasu P, Mani T, Dhingra R. Management strategies for transmigrated mandibular canines: Two case reports and review of treatment options. J Academy Dent Educ. 2025;11:76-81. doi: 10.25259/JADE_16_2024
Abstract
Transmigration of canines, which refers to the repositioning of unerupted/erupted (mandibular) canines across the midline, presents challenges in dental practice. This phenomenon is rare, with an incidence ranging from 0.8% to 3.6%. Two case reports are presented, highlighting the management of transmigrated mandibular canines. A 23-year-old woman with protruding upper front teeth and transmigrated mandibular canines (Type 5 according to Mupparapu classification) was presented in Case Report 1. Treatment involved non-extraction in the maxillary arch, while two options were proposed for the mandibular arch: Removal of both primary canines with surgical exposure of transmigrated and impacted permanent canines either distalizing them to their ideal position or allowing them to erupt in their original position and then reshaping them. A 25-year-old man with transmigrated mandibular canine (Type 5) and spacing in the upper front tooth region were described in Case Report 2. Treatment included extracting the mandibular retained deciduous canine and creating space for the transmigrated canine. The treatment plan prioritized orthodontic alignment over surgical intervention due to patient preference and the rarity of Type 5 transmigration. Both cases underscored the importance of early detection and orthodontic biomechanics in managing transmigrated canines, preserving dental arch integrity, and optimizing facial esthetics and function. Understanding the various treatment options and considering patient preferences are crucial for achieving successful outcomes in transmigrated canine cases.
Keywords
Case reports
Impaction
Mandibular canines
Orthodontic treatment
Transmigration
INTRODUCTION
The repositioning of the canine or the movement of an unerupted canine across the midline is referred to as transmigration.[1] Transmigration primarily affects canines and is more common in females than males. It is more frequently seen in the mandible than the maxilla.[2]
One is more likely to find impacted maxillary canines, but mandibular transmigration is more common. The mandibular canines serve as the “cornerstone” of the dental arch and are crucial for maintaining facial expressions, stable dental structure, and efficient mastication. If this defect is discovered early enough, orthodontic treatment or surgical transplantation may be able to retain these canines.[3] The pre-eruptive migration of unerupted teeth across the midline in the bone is known as transmigration, and it is an incredibly unusual phenomenon. It is uncommon to find this abnormality. Although impacted canines are the second most common type of impacted tooth, with a prevalence of 1–2%, orthodontic treatment still has to address this serious issue. Effective management of these cases requires meticulous planning and cooperation among orthodontists, oral surgeons, and other dental specialists to ensure optimal outcomes for patients.
The most common causes of teeth impaction are avitaminosis, endocrine problems, bone fibrous dysplasia, and genetic factors. Furthermore, the local variables linked to teeth impaction are also linked to transmigration. The direct causes of transmigration include disorders related to resorption and bone apposition, as well as metabolic changes within a specific region of the dental follicle surrounding the canine germ, resulting in a deviation from the normal eruption pathway.[4]
A mandibular canine is considered transmigrated if it has migrated more than half of its length beyond the midline, per Javid.[5] Nonetheless, Joshi[6] believed that a canine’s propensity to cross the mandibular midline suture barrier is more important than how far it migrates. In addition, it usually migrates along its long axis in the direction of least resistance, with the crown taking the lead. The majority of researchers conclude that the main causes of transmigration are the mesioangular and horizontal rotation of tooth buds. Bruszt[7] believes that the canine germ, positioned ahead of the lower incisors, is pushed toward the contralateral side by facial growth. On the other hand, other hypotheses contend that an incorrect eruption could result from an exceptionally high eruption force or from modifications made inside the tooth germ’s crypt. In addition, compared to bilateral transmigration, more unilateral cases were documented. Furthermore, the left canine was more engaged than the right.[3]
Five categories were identified by Mupparapu from transmigrated mandibular canines: [8]
Type I: Canine impacted mesioangularly over the labial, lingual, or midline to the anterior teeth, with the midline being crossed by the crown of the tooth.
Type II: Canine horizontally impacted below the incisor apices, close to the inferior border of the jaw.
Type III: The canine erupted either distally or mesially from the opposing canine.
Type IV: Canine horizontally impacted below the apices of the opposing molar or premolar near the inferior border of the jaw.
Type V: The canine is positioned vertically in the center, and its long axis crosses the midline.
These categories vary in frequency: Type I (45.6%) is the most prevalent, followed by Type II (20%) and Type IV (17%), Type III (14%), and Type V (1.5%).
Howard[9] observed that the impact of axial inclination on the migration patterns of impacted canines is a significant aspect to consider in understanding their movement within the dental arch. Canines that have been impacted and have an axial inclination of 25°–30° to the midsagittal plane are generally displaced rather than migrating across the mandibular midline. This implies that there is not much movement in the other direction toward the dental arch within this region. Canines inclined from 30° to 95° belong to a group that tends to cross the mandibular midline. This indicates that as the inclination angle increases within this range, there is an increased likelihood of migration across the midline. There appears to be a transitional zone between 30° and 50°, where some canines may or may not cross the midline. This implies that the degree of inclination within this range may not consistently predict migration behavior. However, when the axial inclination exceeds 50°, there is a more pronounced tendency for crossing the midline, suggesting a more consistent migration pattern beyond this threshold. In summary, our findings highlight how important it is to take into account the angulation of impacted canines when forecasting their migration patterns. When establishing a course of treatment and determining the probability of midline crossing in Canines, the angle of inclination is a useful measure. Shafer et al., suggestion[10] for canine impaction included the following sequelae:
Malpositioning of the impacted tooth lingually or labially,
Neighboring teeth migration and loss of arch length,
Internal resorption,
Formation of dentigerous cysts,
External root resorption of the impacted tooth and neighboring teeth,
Infection, especially in cases of partial eruption, and
Referred pain and combinations of the aforementioned sequelae.
For mandibular canines that are impacted or transmigrated, a number of treatment options are recommended. These include surgical extraction, exposure followed by orthodontic alignment, intra-alveolar tooth transplantation, and observation. One such method is surgical relocation, which entails preparing the alveolar socket surgically before extracting the impacted tooth and fixing it in the proper location within the dental arch. This approach is often more economical and provides a better option than fixed or removable prosthesis. Generally speaking, patients who practice good dental hygiene are the best candidates for surgical tooth repositioning. The intrusive nature of the procedure and the unknown stability of the results over the long term are disadvantages, though, as there is a chance of root resorption and gingival attachment loss. Timely identification of impacted/transmigrated canines is crucial for initiating prompt intervention to enhance facial symmetry as well as maximize functionality.
CASE 1
The primary complaint of a 23-year-old female patient referred to the Department of Orthodontics and Dentofacial Orthopedics was that her upper front teeth were positioned forward, resulting in an unsightly smile that persisted for 5 years.
An intraoral clinical examination showed that every permanent tooth up to the third molars erupted in the oral cavity, except for lower right and left canines 33 and 43, as well as 73 and 83, which are still retained. 4 mm overjet and 3 mm overbite were recorded. Molar relation was Angle’s class I on both sides with bimaxillary protrusion [Figure 1].
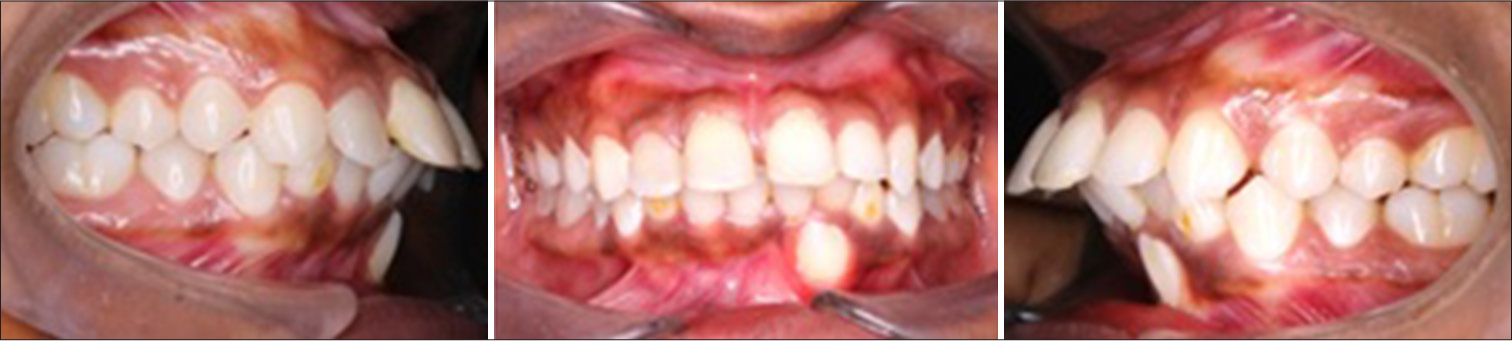
- Intraoral photograph – Case 1.
No relevant medical history was found; however, the patient’s dental history indicates that they had a traumatic fall and had undergone root canal treatment in 11, 12 10 months before, and now, the patient is completely asymptomatic in 11,12.
Orthopantomograph examination
A well-defined hyperdense structure with central linear hypodensity is noted in between roots of 31 and 41 regions resembling morphology of mandibular canine – transmigrated 43 – Type 5 transmigration of 43 as per the classification given by Mupparapu.
Root apices of mandibular canines that were transmigrated are seen 2.6 mm above the lower border of the mandible.
-
A well-defined hyperdense structure with central linear hypodensity is noted in between roots 32, 73, and 34 region where the coronal aspect is in contact with the labial aspect of 32 and mid portion is in contact with 73 regions and the apical part is in contact with the apex of 34 regions – impacted 33 [Figure 2].
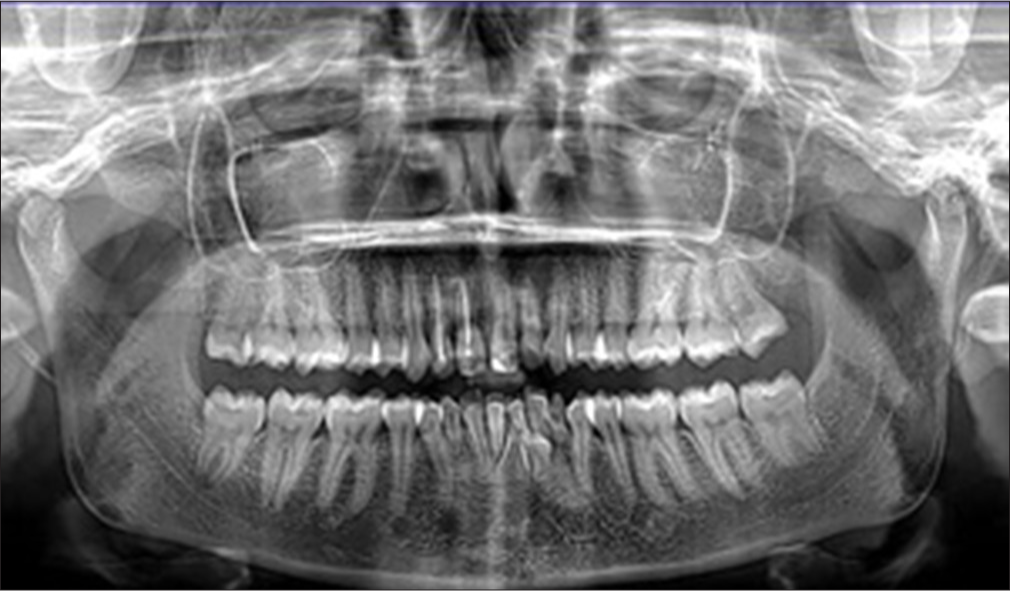 Figure 2:
Figure 2:- Orthopantomograph – Case 1.
It is in close contact with the roots of the 34, 32, and 31 regions.
Cephalometric findings [Figure 3] show skeletal class 1 base with (ANB = 1.6°, SNA = 80.4°, SNB = 78.7°), severe dentoalveolar protrusion (interincisal angle = 87.5°), and hypodivergent mandibular plane angle (SN-MP = 28°, FMA = 17°).
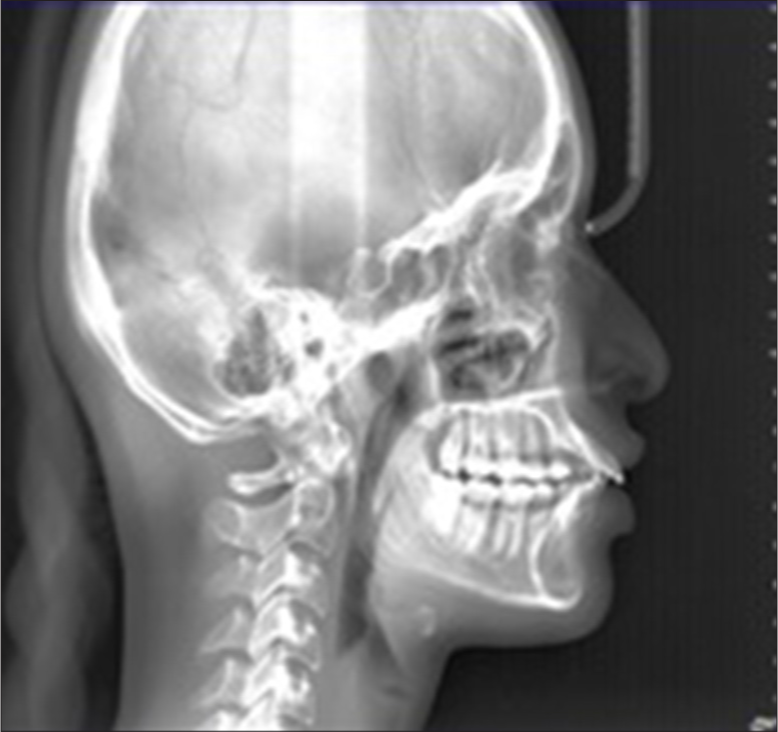
- Lateral cephalogram – Case 1.
Figure 4 shows the cone beam computed tomography (CBCT) image of the canine, and as seen in the sagittal view, the lower left permanent canine (33) is placed buccal to the roots of the 32 region. The lower right permanent canine (43) is vertical and placed buccal between the roots of 31 and 41.
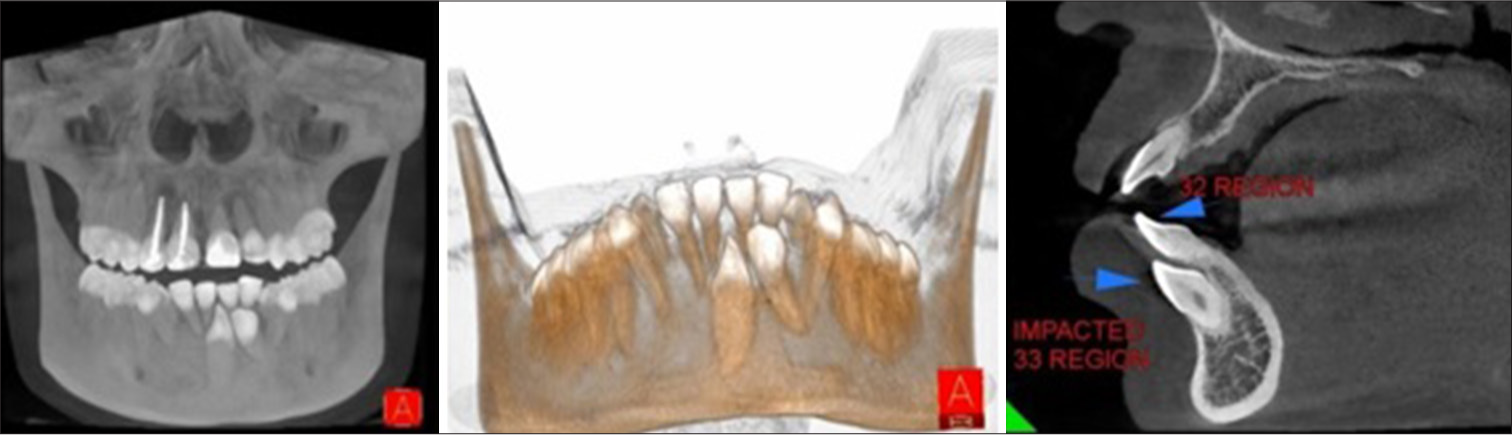
- Cone beam computed tomography images – Case 1. Blue arrow above indicates impacted 32 and below indicates impacted 33 region
The patient was given two treatment choices for the mandibular arch, while the maxillary arch was to be treated non-extraction first, then leveling and alignment. The first plan was to extract the deciduous canines 73 and 83 and maintain these spaces followed by surgical exposure of 43 and then distalizing the lower right and left canines into their ideal position and then bringing them into proper arch alignment.
The second treatment plan was to extract both the primary canines followed by distalizing the permanent incisors into the space created and then bringing the lower right permanent canine (43) in the place of 41 as well as the lower left permanent canine (33) at the place of 32, which has to be further followed by reshaping of the required teeth for proper esthetics and smile.
The patient opted for the third treatment plan of extracting the deciduous canine and the impacted canine 43 followed by distalizing 33 to its ideal position occupying the space created by the extraction of deciduous canine [Figure 5]. Due to the poor prognosis of the other treatment plan and the expected disadvantages such as long duration of treatment and fenestration during distalizing transmigrated canine into their ideal position across the midline.
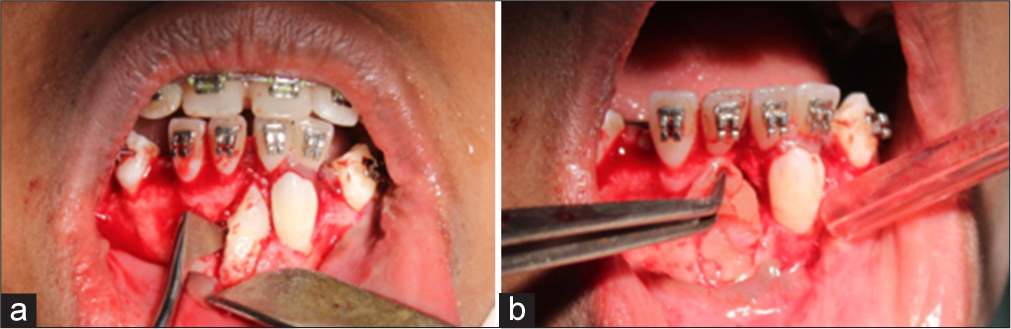
- (a) Extraction of transmigrated canine, (b) Placement of PRP. PRP: Platelet rich plasma-Case 1.
CASE 2
A 25-year-old aged male patient reported with a primary problem of spacing in the maxillary anterior teeth for 10 years. He also complained that he noticed a small white-colored bulge in his lower left front teeth region for 2 years. No relevant medical history was found. It was his first dental visit.
On intraoral examination, all permanent teeth erupted till the third molars except 28 which were missing. Microdontia was noted in 18. Overjet and overbite were recorded as 4 mm each. Molar relation was Angle’s Class 1 on both sides and canine relation was Class 1 on the left side and not established on the right side [Figure 6]. OPG examination reveals Type 5 transmigration of 43 according to the Mupparapu classification [Figure 7]. The transmigrated tooth was not accompanied with any pathologic findings.
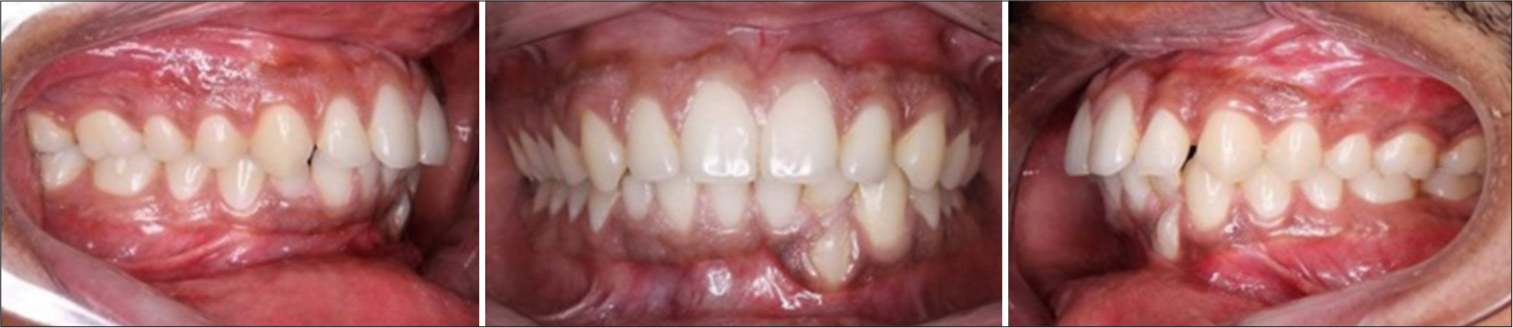
- Intraoral photograph – Case 2.
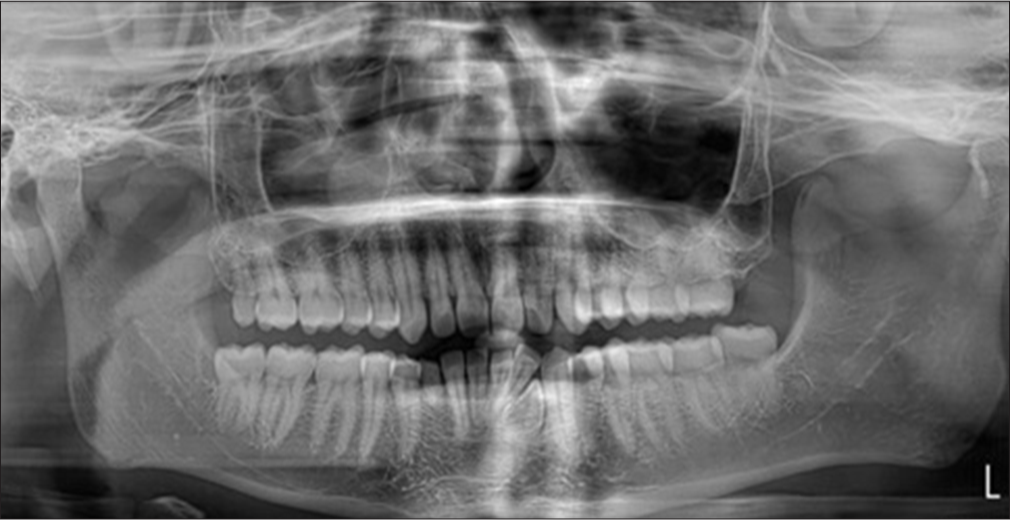
- Orthopantomograph – Case 2.
Cephalometric findings [Figure 8] show Skeletal Class II base with ANB = 4° (SNA = 82°, SNB = 78°) with hypo-divergent growth pattern with Go-Gn – SN = 24°, FMA = 20°, Jarabak’s ratio = 74%, and proclined incisors with IMPA = 114° and interincisal angle = 113°. CBCT [Figure 9] shows buccally placed transposed 43 between the roots of 42 and 43.
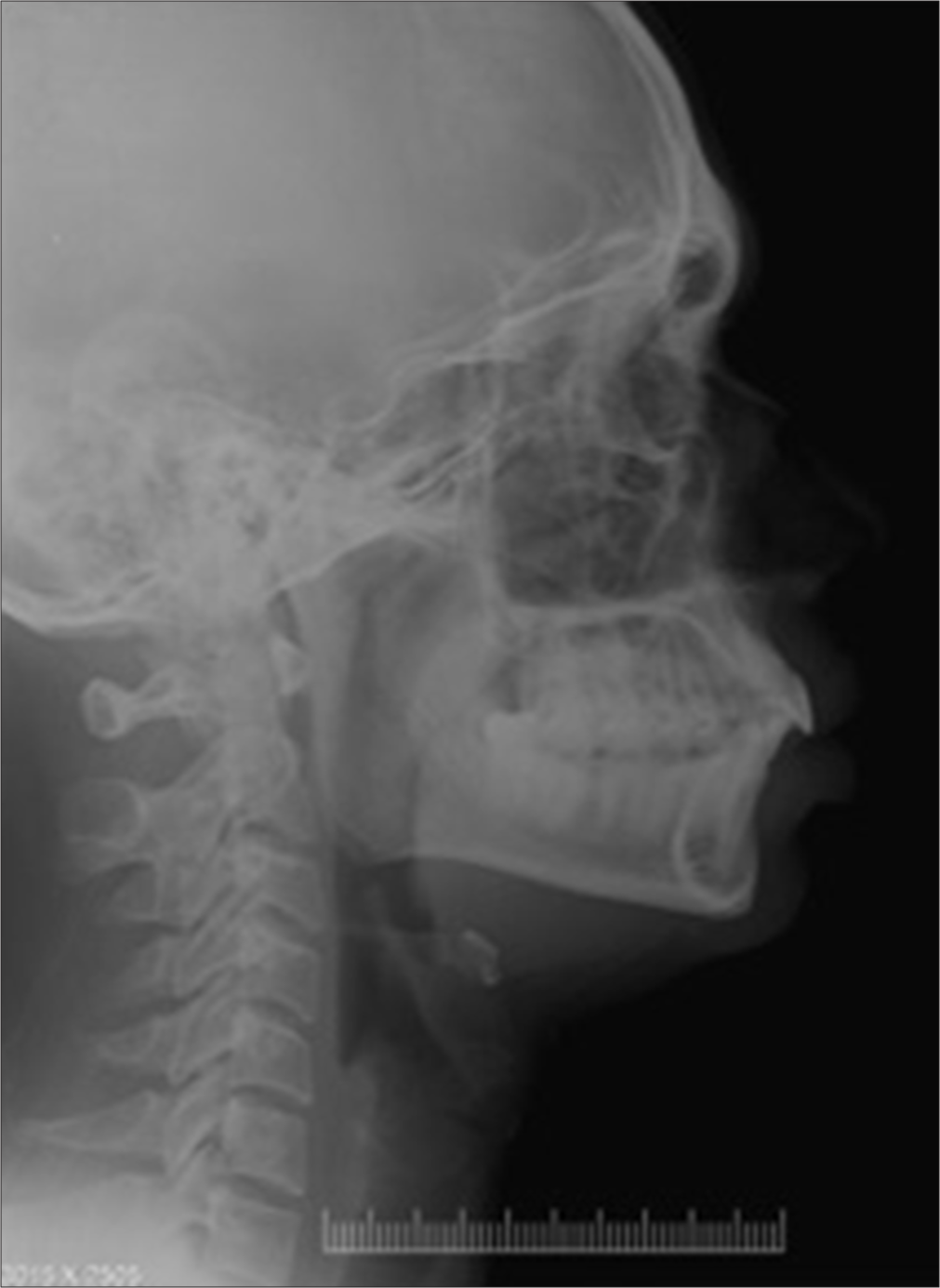
- Lateral cephalogram – Case 2.
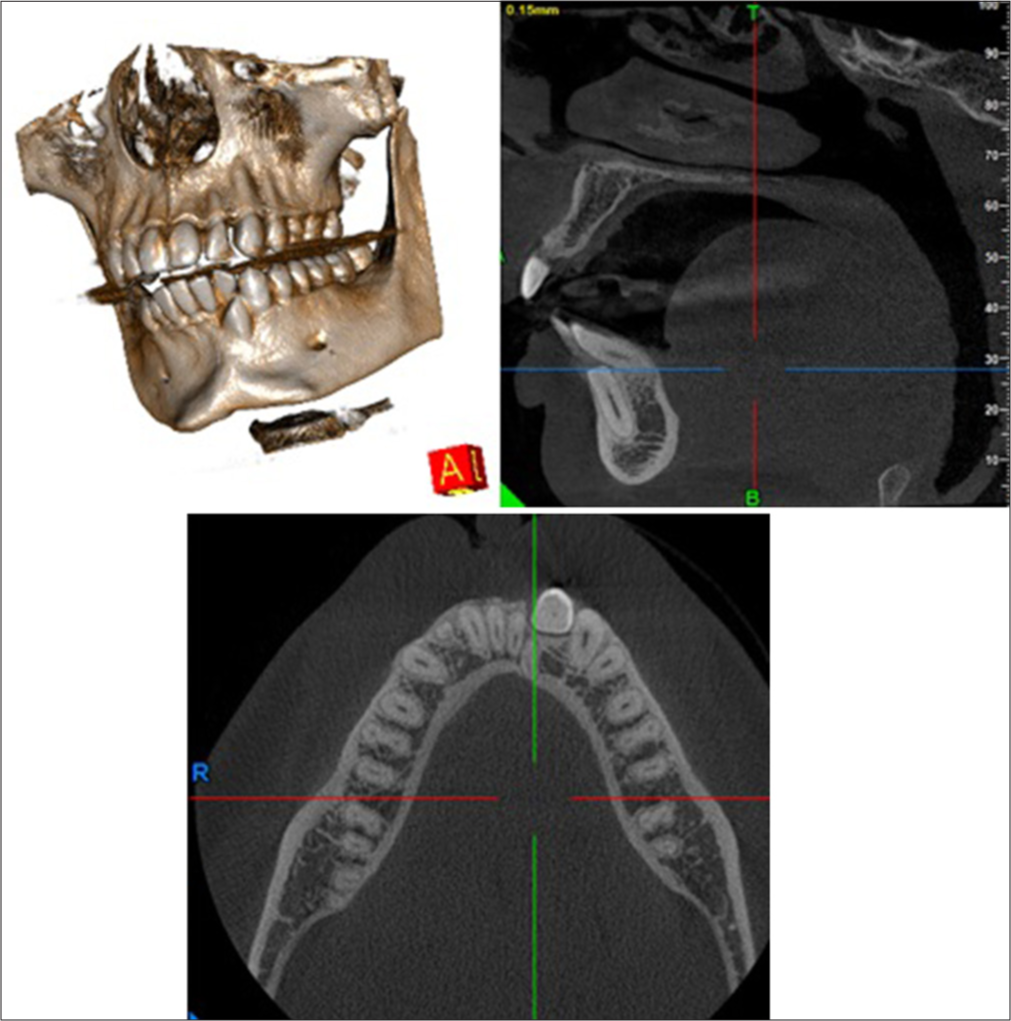
- Cone beam computed tomography images – Case 2.
The treatment plan called for non-extraction in the maxillary arch followed by leveling and aligning, whereas for the mandibular arch is to extract the retained deciduous canine 83 followed by leveling and aligning using the space created by the extraction of 83 followed by surgical exposure of impacted 43 and bringing it into the arch in the position between 32 and 33 followed by reshaping of 43 as per esthetic and functional requirements. Patient accepted this treatment plan due to the favorable prognosis and there is no tooth movement across the midline.
DISCUSSION
There are very few reports of dental transmigration in mandibular canines. There have been reports of incidences ranging from 0.1–3.6% to 0.8–3.6%.[5,6] In their investigation on the frequency of transmigration of different mandibular teeth, Kara et al.[11] found that the incidences for transmigrating mandibular canines were 0.079%, transmigrant lateral teeth were 0.0017%, and transmigrant premolars were 0.0026%. Depending on their position and biological circumstances, unerupted transmigrated mandibular canines have several options for treatment. They could entail orthodontic, surgical, and cosmetic dental procedures.
Four options for treating such a condition have been documented in the literature over the years: (1) Orthodontic traction, (2) surgical extraction, (3) radiographic monitoring, (4) auto-transplantation.
According to cases reported by Watted et al.[12] and Mesquita and Salgado,[13] space closure was suggested after the transmigrated lower canine was surgically removed. Transplantation may be done if the mandibular incisors are in their natural positions and there is enough space for the transmigrated canines. Cases of transplanted mandibular canines that were transmigrated were described by Kulkarni and Lee[14] and Verma et al.[4] According to Ando et al.,[15] the maximum amount of transmigratory canine migration occurs faster before the establishment of its root.
In the present case reports, both the transmigrated canines are under Type 5 Mupparapu classification whose incidence is also very low (1.5%). Therefore, the plan consisted of doing minimal interventions as the patients were also not willing for any major surgical procedure. After the odontoma was removed and the associated canines were surgically exposed, Taguchi et al.[16] found an improvement in their position.
CONCLUSION
In managing transmigrated canines and smile designing, the amount of prosthetic and surgical intervention required can be reduced with appropriate diagnosis and use of orthodontic biomechanics. The core components of the dental arch are thought to be canines. They are crucial for preserving the harmony and functionality of the face.
In the present case reports, the treatment plan for the transmigrated canines was to orthodontically align them in the spaces present rather than doing any surgical procedure to reposition them in the arches.
In general, the unerupted or transmigratory canines exhibit no symptoms. Panoramic radiographs are typically needed to diagnose transmigrated canines, and radiographic evaluation is crucial for diagnosing impacted canines. Better appearance and function can be achieved by preserving these teeth, the surrounding tissues, and the dentition by prompt detection and treatment.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship: Nil.
References
- Transmigration of non erupted mandibular canines: Report of cases. J Am Dent Assoc. 1971;82:1395-7.
- [CrossRef] [PubMed] [Google Scholar]
- Transmigration of mandibular canine-case report. Polish J Radiol. 2014;79:20.
- [CrossRef] [PubMed] [Google Scholar]
- Transmigration of mandibular canines. Case Rep Dent. 2013;2013:697671.
- [CrossRef] [PubMed] [Google Scholar]
- Management of a transmigrated mandibular canine. J Orthod Sci. 2012;1:23-8.
- [CrossRef] [PubMed] [Google Scholar]
- Transmigration of impacted mandibular cuspids. Int J Oral Surg. 1985;14:547-9.
- [CrossRef] [PubMed] [Google Scholar]
- Transmigrant mandibular canines: A record of 28 cases and a retrospective review of the literature. Angle Orthod. 2001;71:12-22.
- [Google Scholar]
- Neurological anomaly associated with extreme malposition of a mandibular canine. J Oral Surg (Chic). 1958;11:89-90.
- [CrossRef] [PubMed] [Google Scholar]
- Patterns of intraosseous transmigration and ectopic eruption of mandibular canines: Review of literature and report of nine additional cases. Dentomaxillofac Radiol. 2002;31:355-60.
- [CrossRef] [PubMed] [Google Scholar]
- Analysis of different type of transmigrant mandibular teeth. Med Oral Patol Oral Cir Bucal. 2011;16:335-40.
- [CrossRef] [PubMed] [Google Scholar]
- Transmigration of impacted canines: A report of two cases and a review of the literature. J Dent Sci. 2014;12:23-32.
- [Google Scholar]
- Transmigrant mandibular canine-case report. Rev Port Estomatol Med Dent Cir Maxilofac. 2015;56:63-7.
- [CrossRef] [Google Scholar]
- Vital autotransplantation and orthodontic treatment of a transmigrant mandibular canine. Pediatr Dent. 2016;38:1-4.
- [Google Scholar]
- Transmigration process of impacted mandibular cuspid. J Nihon Univ Sch Dent. 1964;6:66-71.
- [CrossRef] [Google Scholar]
- Eruption disturbances of mandibular permanent canines in Japanese children. Int J Paediatr Dent. 2001;11:98-102.
- [CrossRef] [PubMed] [Google Scholar]






