Translate this page into:
A rare case report of mandibular spur on inferior border of the mandible – “Note the point”

*Corresponding author: Mathew Jacob, Associate Professor, Department of Oral Pathology and Oral Microbiology, Vinayaka Mission’s Sankarachariyar Dental College, Vinayaka Mission’s Research Foundation (Deemed to be University), Salem, Tamil Nadu, India. docere_mathew@yahoo.co.in
-
Received: ,
Accepted: ,
How to cite this article: Mohammed ZD, Jacob M, Fenn SM. A rare case report of mandibular spur on inferior border of the mandible – “Note the point.” J Academy Dent Educ. 2023;9:97-9. doi: 10.25259/JADE_27_2023
Abstract
Bone spurs are projections that are seen along the borders of bone. These pathologies are usually located within joints and are referred to as osteophytes. Due to the increased frequency or incidence within the joints, osteophytes are named after the location of occurrence, such as extraspinal osteophytes. Due to the lack of a definition or classification of bone spurs in scientific literature and the paucity of cases reported in the jaws, the the current article reports a case of the bone spur along the inferior border of the mandible.
Keywords
Bone spur
Mandibular spur
Osteophyte
INTRODUCTION
Bone spurs are bony projections along the borders of bone. These are also called as osteophytes due to its prevalence in joint spaces and have been identified as early manifestations of arthritis.[1] The bony outgrowth in the current case report, which was similar to those seen in osteophytes affecting other parts of the body, was found along the inferior border of the mandible rather than in a joint space. As a result, the word “bone” or “mandibular spur” is rendered for the present case, and the case report is presented due to the rarity of cases in the scientific literature.
CASE REPORT
A 19-year-old male patient presented to the oral medicine and radiology department with the chief complaint of a point-like hard mass along the lower border of the right mandible. The patient did not provide a history of any recent trauma or recall any significant childhood injuries. There were no other abnormalities observed during the intraoral examination. Extraoral examination revealed a 3 × 5 mm bony hard “pointed” swelling along the lower border of the right mandible [Figure 1a]. The patient was previously unaware of such swelling, and as an adult male, he did not notice the swelling during routine facial grooming. Based on the history and clinical findings, a provisional diagnosis of normal bone variation was made.
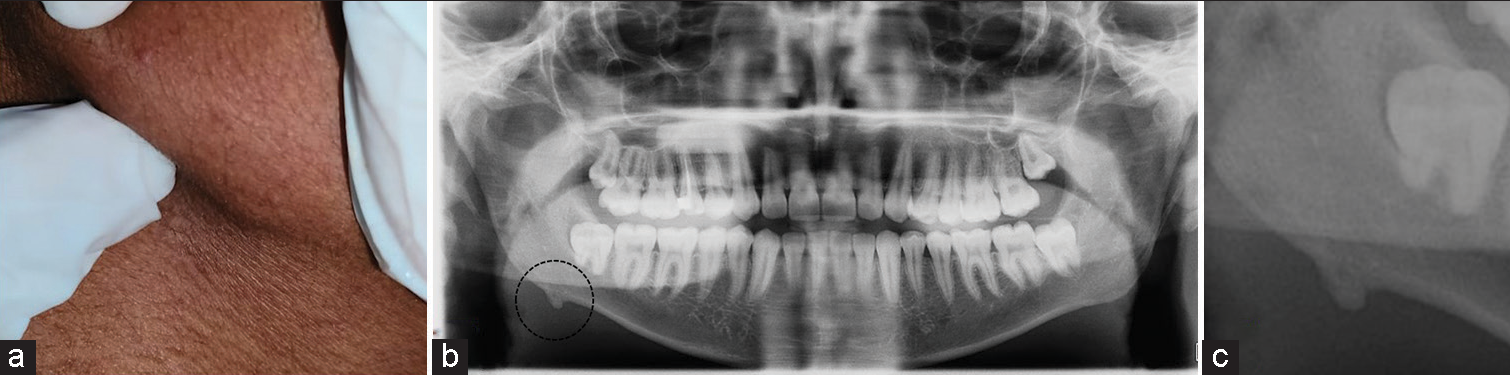
- (a) Clinical photograph showing the bone spur along the inferior border of mandible, (b) orthopantomogram, and (c) magnified view.
An orthopantomogram (OPG) was taken to rule out any osteogenic disease or generalized bone pathology. The OPG revealed a sharp conical elevation along the lower border of the right mandible. The elevation had the same density as the adjacent bone with a border with the same intensity as the cortical bone [Figure 1b-c]. Since the conical mass appeared inert in the radiograph and did not cause any functional difficulty or esthetic change, no additional radiograph or biopsy was considered at this point. However, the patient was advised to report if any change in size or shape of the swelling or experience pain or paresthesia.
DISCUSSION
Bony swellings on the face are alarming for most patients, especially in the younger age group, as they can indicate many diseases from congenital to neoplastic entities. When first encountered by palpation, these can usually be suspected to have occurred due to trauma during childhood or recently. In the present case, the male patient reported small sharp or conical bony hard swelling along the inferior border of the mandible. The swelling was noted when having felt his hands over the inferior border of the mandible and was not evident during shaving which had alarmed the patient. Scientific literature on such pointed outgrowth on the face or jaws is limited to one case report by Curtis et al. associated with Cornelia de Lange syndrome in the year 1977 with radiographic resemblance to the spur mentioned in the case report.[2]
In the present case report, the location of the bony outgrowth was approximately 1.5 cm away from the angle of the mandible and coincides with the attachment of masseter muscle. Another interesting feature was the shape of the outgrowth which was conical with a blunt apex and the long axis was directed anteriorly. The significance of mentioning the direction of growth is that the present outgrowth resembled osteophytes seen in joint spaces, with the tendency to grow along the direction of the pull of the attachment tendon. However, no additional radiographic investigations were done due to the lack of any signs or symptoms of discomfort or pain. Furthermore, the OPG had shown that the growth was benign and had the same density as adjacent bone, and thus, other radiography was not indicated, also to avoid untoward exposure to radiation. Exostosis or tori, based on the site, is the most common condition to consider in the differential diagnosis. Tori are developmental anomalies that manifest as large rounded smooth protuberances covered by normal oral mucosa on the lingual aspect of the mandible. On clinical examination, the current case presented as a single, small, sharp, and angulated bony protrusion positioned along the inferior border of the mandible with the tapering fashioning the pull of the tendon and, therefore, was not considered in the final diagnosis.[3]
The purpose of the case report is to increase awareness about the incidence of these entities that can be included in classifications of bone and joints of the head and neck as either normal variation or, in fact, analogous to the bone spurs that develop in other parts of the body. Close monitoring and follow-up, as with bone lesions, is mandatory to carefully observe the changes with age as well as due to the paucity of scientific literature on such entities.
CONCLUSION
Anomalies arising from the bone are abundant that are classified as developmental, reactive, or neoplastic in nature and careful diagnosis with appropriate radiographic investigations is required in diagnosis, treatment planning, and monitoring. The present case is intriguing as it describes a bone outgrowth which clinically and radiographically resembles osteophytes developing in joints. The literature review identifies only one case report which is similar to the present case. The current case report describes a unique finding that can be taken into consideration due to the dearth of case reports on such bony outgrowths or and possible inclusion as classifiable entities of bone lesions of the head and neck.
Ethical approval
The research/study complied with the Helsinki Declaration of 1964.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
Financial support and sponsorship
Nil.
References
- Review article: Osteophytes. J Orthop Surg (Hong Kong). 2016;24:403-10.
- [CrossRef] [PubMed] [Google Scholar]
- Spurs of the mandible and supracondylar process of the humerus in Cornelia de Lange syndrome. AJR Am J Roentgenol. 1977;129:156-8.
- [CrossRef] [PubMed] [Google Scholar]






