Translate this page into:
Magnetic mallets – A stroke of luck in implantology: A review
*Corresponding author: N. Vidhyasankari, Department of Prosthodontics and Crown and Bridge, KSR Institute of Dental Science and Research, Namakkal, Tamil Nadu, India. drvidhyasankari@ksridsr.edu.in
-
Received: ,
Accepted: ,
How to cite this article: Visale K, Manimala V, Vidhyasankari N, Shanmugapriya SV. Magnetic mallets – A stroke of luck in implantology: A review. J Acad Dent Educ 2021;7(1):6-9.
Abstract
Magnetic mallet was introduced in dentistry by Bonwill in 1873. It was introduced with the aim of increasing the efficacy of hammered gold fillings. Magnetic mallet is a magnetodynamical handpiece with an ergonomical design. It comprises central control with force adjustment, sterilizable handpiece with different replaceable tips, and pedal control. It comes with an entire range of bone expanders/osteotomes, cutter, and other instruments. It is applicable for procedures such as tooth and root extraction, impacted tooth removal, delayed implant placement, bone manipulating and sinus lifting procedures, root apex resection, removal of crowns, bridges, and implant part. The use of magnetic mallet is said to provide with better clinical advantage.
Keywords
Mallets
Osteotomes
Sinus lift
Dental implants
INTRODUCTION
Research and innovation in oral implantology is a never ending process. Over the years, various newer technologies have been developing in the field of oral implantology. One such innovation is the introduction of “magnetic mallets.”[1] Bonwill patented dental magnet in 1873 and was the first to in stomatology. It was introduced with the aim of increasing the efficacy of hammered gold fillings, which would be achieved by continuous and even mechanical hitting of mild intensity. Hence, a better precision in hammering gold fillings would be possible.[1] Crespi in 2012 first described the use of magnetic mallets in oral implant procedures.[2]
Osteotomes are an integral part of oral implantology. They are used for various procedures such as osteotomy preparation for implant placement, sinus floor elevation, ridge splitting, and also for extractions.[3] Use of osteotomes is not new in dentistry. To overcome the disadvantages of the conventional sinus lift procedure by the lateral approach, Summersin, 1994, proposed a conservative approach using a set of osteotomes.[1] However, the use of osteotomes is generally a procedure with poor patient compliance due to the inconvenience caused to the patients because of the tapping motion. In such a juncture, the introduction of magnetic mallets can be considered as an innovation which is said to provide with better working standards.
DESIGN OF MAGNETIC MALLETS
The magnetic mallet is a magnetodynamical handpiece with an ergonomical design [Figure 1].[4] It comprises a central control unit in which adjustments are provided for altering the forces of mechanical blows.[5] It comes with a sterilizable handpiece joined to the control unit with a cable.[4] Furthermore, different replaceable tips can be fitted into the handpiece based on the procedure being performed. A pedal control is provided for operating the mallet. The current magnetic mallets provide four different force adjustments, that is, 75, 90, 130, and 260 kp.[1]

- Magnetic mallet.
ATTACHMENTS
The magnetic mallets come with an entire range of bone expanders/osteotomes, cutters, and other instruments intended for specific procedures. They are available separately as well as within autoclavable trays. All instruments are made of surgical grade 630 stainless steel which are passivated and tempered to ensure their longevity.[4] Different kits are available such as osteotome kit, extraction kit, and ridge split kit. Each instrument kit contains both straight and double bend instruments, facilitating use in the posterior regions also.[6] A separate crown remover handpiece is also available which can be used with the regular magnetic mallet base power unit.[1]
COMPARISON WITH TRADITIONAL OSTEOTOMES[1]
It is to be noted that the maximal force of traditional handpieces is 40 kp and the magnetic mallets provide up to 6–7-fold increased force compared to the traditional ones. Even though the magnitude of force applied with magnetic mallets is much greater than conventional osteotomes, it is less damaging to the patients. Hence, the magnetic mallets are far less invasive, due to the fact that the 350–400 μs occur with traditional mallets to give a fast blow whereas this duration for magnetic mallets is reduced to 1/4th or 1/5th of its time. The impulse of blow takes only 80–100 μs with the magnetic mallets. Therefore, in spite of a greater force being applied, the extremely short time of force application drastically reduces the discomfort to the patients.
In procedures using traditional mallets, the hitting force may dislocate the auditory ossicles resulting in dizziness after the surgery. Hence, there is an increased risk for the patients to develop benign paroxysmal positional vertigo. The incidence of benign paroxysmal positional vertigo is reported using hand mallets and may be due to the inertia produced by skull due to fast impulses. This consequence can be avoided with the use of magnetic mallets. Major part of blow force is directed to the plastic change of the bone site being worked on and only a small portion of the force moves the skull. This is opposite in case of traditional osteotomes, where a greater amount of force is directed in moving the skull and only minimal force is used up for bone manipulation, thus reducing the efficiency of the procedure.
ADVANTAGES OVER CONVENTIONAL INSTRUMENTATION
The magnetic mallets provide various advantages for both patient and the clinician.
Magnetic mallet has a control of strength and time of application.[7]
Mallets aid in atraumatic extraction of tooth, thereby leading to minimal or no use of bone grafts. Hence, it is cost-effective too.[8]
Extractions can also be done faster and atraumatically
Magnetic mallet produces high powerful energy with high acceleration applied in a short time[7]
During the preparation of osteotomy site for implant placement, no drilling is requited. Therefore, heat damage and removal of bone do not happen. Instead, the bone gets condensed around the implant site helping in faster osseointegration
Procedures such as impaction removal and ridge splitting can also be done faster
Sinus lifting procedures are also made easy, because as the sinus membrane elevates, bone is also condensed, paving way for immediate implant placement with better primary stability and little or no use of biomaterials
The mechanical friction between the instrument and bone takes place within microseconds. This time frame is insufficient to increase bone temperature
There is no heat generation with magnetic mallets, hence, no irrigation is required. Due to irrigation, the bone minerals required for ossification get washed away. However, this does not happen with magnetic mallets
Unlike piezo, where inserts need to be replaced after 10–15 procedure, the magnetic mallet inserts last relatively longer
Magnetic mallets have advantages of both physiodispenser and piezo unit
The ergonomics of the handpiece allows the clinician to use only one hand for positioning the instrument in the intended site
Shock wave generated by magnetic mallet was of 130 DaN with a light point of 80 μs. The bone plastic deformation was thus greatly facilitated and enabled the total energy absorption so that a minimal and negligible acceleration on the jaw mass remained[7]
As no irrigation is required and only one hand is needed for use, there are no obstructions hindering the clinician view of the operating site. As an advantage, the instruments depth of penetration can be easily monitored and controlled
When using magnetic mallets, the forces are delivered in a precise, constant, and predictable manner. Hence, the clinician can have better control while performing the procedure
Better access in possible in the posterior maxilla with the use of curved inserts
Procedures are less invasive leading to faster patient recovery.
MODE OF ACTION
The handpiece is powered by a control unit. It makes use of an electromagnetic field. The axial and radial movements produced by shock waves are transmitted to the osteotome tip and have greater potential than the conventional mallets. An electronically operated collision occurs between two masses which provide a high intensity impact. The elastic wave produced, followed by a certain amount of motion, creates an inelastic shock wave on the bone.
RESULTS IN IMPLANTOLOGY[1]
Moderate shake of skull occurs when compared with the traditional mallet osteotome.
No consequent headaches, drowsiness, dizziness, or nausea.
Deviation from desired direction during osteotomy may occur with the differences of bone density and is avoided using magnetic mallets.
Magnetic mallets are operated by single hand due to better visualization of operating field [Figure 2].[4]
Faster bone healing as more viable living bone present.
The alveolar bone is only parted and drilled but not shaved. This preserves more bone at the preparation site.[8]
Double-curved tips, adds more accessibility for osteotomy at any part of the oral cavity.
Bone splitting can be carried out easily and precisely in case of thin alveolar bone.
Bone condensation by widening and thickening of osteocytes take place with no debris.
No heat production on drilling where cooling fluid is not needed. Hence, physiological substances are not washed out along the bone debris and the living bone substances are left out which promote healing.
Use of magnetic mallets serves as minimal invasive surgery thereby reduces the post-surgical pain for the patients.
The application of magnetic mallet is gentle as it works under precise calibrated force with short impulses, depth, and duration.
Bone split for thin alveolar bone and sinus lift can be performed easily. A combination of other techniques and instruments such as piezo electric, laser, drills, scalpels, and bone cutters is used.
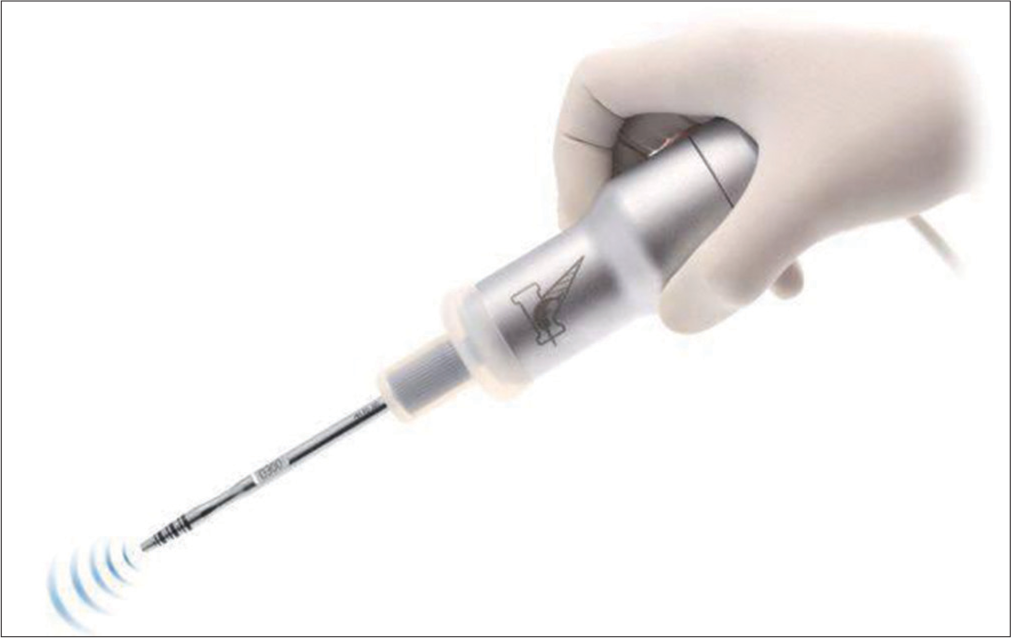
- One handed operation of magnetic mallets.
CLINICAL EVALUATION[9]
No pre-clinical complication
No clinical intraoperative complications such as instrument fractures, dislocation, and injury to vital anatomical structure
No post-clinical side effects such as post-surgical site pain, headache, paroxysmal vertigo, or other discomfort.
DISCUSSION[1]
The uses of magnetic mallets in dental field are vast including tooth and root extraction, impacted and retained tooth/ root removal, extraction followed by immediate implant placement, bone manipulation procedures such as bone expansion, bone condensation and ridge splitting and removal of crowns, bridges, and implant parts.[10,11]
The success of implantology is greatly dependent on the bone density and magnetic mallet played an important role in changing the era of dental implant dentistry.[12]
Following tooth extraction, atrophy of alveolar jaws at different rates both volumetrically and qualitatively begins. Good prognosis of implants in dense bone than in the soft bone is much reported in literature. The anchorage of implants in atrophied alveolar ridges with varied shapes and density is jeoparadized and results in failure of dental implants.
Maintaining the two parameters, namely, the volume and quality ensures for implant success in a greater ratio.
Hence, sufficient bone density with adequate bone volume is important factors for achieving better anchorage for primary and secondary stability could not be overruled. D3 trabeculae are weaker than D2 trabeculae by approximately 50% and are often found in anterior maxilla, posterior maxilla, and posterior mandible. The bone-implant contact of D3 trabeculae is comparatively less favorable to D4 trabeculae and the width of D3 anterior maxilla is lesser than the anterior mandible. All these facts amplify the failure rate in dental implants, especially in resorbed or soft bone, and therefore, it is a prime mandatory to preserve the existing native bone. Osteotomes and magnetic mallets are beneficial in compression and manipulation of bone and are mandatory in preserving the existing bone.[3] Magnetic mallet helps in lateral compression of bone during osteotome technique as it uses series of gradual increasing tapered instruments and do not generate heat. These are the major factors in determining the far better osseointegration success than an osteotomy in conventional way. As an added advantage, there remains an improvement in bone density both qualitatively and quantitatively and consequently converse D3 bone to D2 bone and D4 bone to D3 bone by condensation. Good dental implant success rate was observed using malleting technique in deficient alveolar ridges with highly reduced bone width and height individuals.
CONCLUSION
The use of magnetic mallets is said to provide with better clinical advantages than the conventional instruments. It is fast, precise, and efficient in bone condensing and suitable instrument for preparing a superior fresh socket for implant placement with simultaneous sinus elevation procedure. More clinical studies are required to validate the use of the magnetic mallets as a safer alternative in oral implant procedures.
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Extraction followed by implant placement using magnetic mallet: A case report. Int J Med Res Rev. 2016;4:1046-8.
- [CrossRef] [Google Scholar]
- Osteotome technique: A minimal invasion way to increase bone for dental implant placement in the posterior maxilla and prevent sinus membrane perforation for single and multiple teeth replacements. J Med Clin Res Rev. 2019;3:1-6.
- [CrossRef] [Google Scholar]
- Available from: https://www.dentalenterprisesllc.com [Last accessed on 2021 Jun 06]
- Available from: https://www.swedenmartinainc.com/en_us/product/implantology_and_surgery17212/equipment_and_special_instruments-17218/magnetic_mallet-17254.html [Last accessed on 2021 Jun 06]
- Available from: https://www.indiamart.com/proddetail/magnetic-mallet-21425158312.html [Last accessed on 2021 Jun 06]
- Available from: https://www.dentalxp.com/vendordetails.aspx?id=390 [Last accessed on 2021 Jun 06]
- Available from: https://www.youtu.be/e0kucwgqzt0 [Last accessed on 2021 Jun 06]
- Electrical mallet in implants placed in fresh extraction sockets with simultaneous osteotome sinus floor elevation. Int J Oral Maxillofac Implants. 2013;28:869-74.
- [CrossRef] [Google Scholar]
- Use of magnetic mallet in bone shaping and implantology. A technical report. Ital J Dent Med. 2019;4:16-30.
- [Google Scholar]






